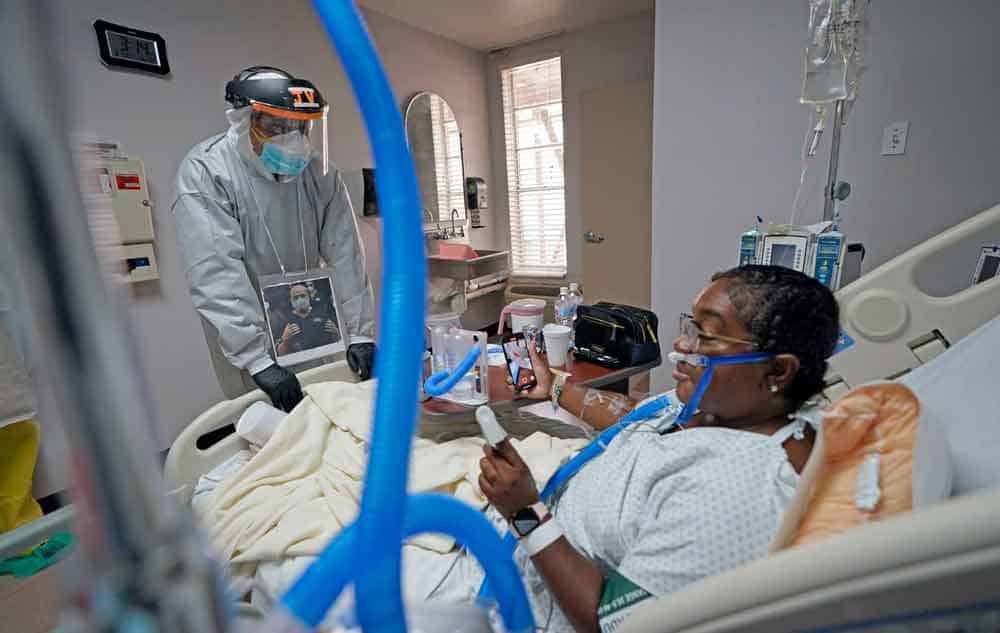
Here are Some Summary Articles about Post-Covid Syndrome
It's Not In Your Head. You Are Experiencing Real Physical Symptoms From A Real Physical Condition.
Here’s what we know so far about the long-term symptoms of COVID-19
By Peter Wark | The Conversation | July 27, 2020
Sufferers with mild illness might expect to get better after a few weeks. But there’s mounting evidence this isn’t the case, and COVID-19 may leave a long-lasting impression on its victims – not just the most severely affected or the elderly and frail.
I'm a Covid-19 'long-hauler'. For us, there is no end in sight
By Jemma Kennedy | The Guardian | July 26, 2020
"As a writer, I spend my days trying to craft believable, satisfying narratives. But as a Covid-19 “long-hauler”, I have given up trying to find an internal logic to the story of my illness. As we now know, thousands of people are suffering a range of bewildering and debilitating post-Covid symptoms that don’t follow any predictable act breaks or intervals."

COVID-19 infections pose a risk of long-term problems like chronic fatigue and other complications
By Damon Cronshaw | Newcastle Herald | July 26, 2020
"Some people who catch COVID-19 have reported experiencing debilitating symptoms for weeks. In some cases, these symptoms have continued for more than two months. Some have categorised these symptoms as a form of chronic fatigue syndrome."
Symptoms like cough and fatigue linger as long as three WEEKS for one in five healthy Americans aged 18 - 34 who catch coronavirus, CDC reveals
By Natalie Rahhal } Daily Mail Australia | 25 July, 2020
"One in five US adults under 35 who contracted coronavirus still had at least one lingering symptom of the virus up to 21 days after they tested positive, a new Centers for Disease Control and Prevention (CDC) report reveals."
Some COVID-19 survivors still have symptoms months after contracting virus, doctors don't know why
By Gina Silva | Fox 11 Los Angeles | July 23, 2020 |
"Most people with COVID-19 recover after two weeks but some have been struggling with this virus for months and they say doctors don’t know what to make of it."
'There are days when I worry this is never going to go away': Living with COVID-19 for the long haul
By Elizabeth Payne | Ottawa Citizen (Canada) | July 22, 2020
“There are still days when I worry that it is never going to go away and that we are always going to be bearing the marks of this on our bodies somehow.”
'Pitch Perfect' Actress Anna Camp Reveals Coronavirus Diagnosis, Has 'Lingering Symptoms' a Month Later
By Lexy Perez | Billboard | July 22, 2020 |
"The panic of contracting a virus that is basically untreatable and is so new that no one knows the long term irreparable damage it does to your immune system is unbelievably stressful. Completely losing my sense of smell and taste without knowing when or even if they will return is extremely disorienting,"
Oakville woman sick with COVID-19 for four months
By Liz Braun | Toronto Sun (Canada) | July 22, 2020
"Susie Goulding is sick and tired of COVID-19. Literally.
Goulding has been sick — and exhausted — for 18 weeks and is what’s known as a “long-hauler” in the COVID-19 battle. She spends her days feeling weak, dizzy and without energy and experiencing what she calls brain fog — she can’t think straight."
COVID-19 Survivors Find Support for Lingering Symptoms in Massive Facebook Group
By Inside Edition Staff | Inside Edition | July 22, 2020 |
"Listening to other people's stories, it makes you feel heard," one of the members said. "We are a community that actually is able to help each other," said another.
Brain fog, fatigue, breathlessness. Rehab centers set up across Europe to treat long-term effects of coronavirus
For much of Europe, the peak of Covid-19 infections has passed. But while hospitals are no longer awash with acute cases, there are thousands of people who had either confirmed or suspected Covid and, weeks or months later, say they are far from fully recovered.
'It completely reframes your life': The people who have had coronavirus but are suffering long lasting effects
ITV (UK) | July 21, 2020
"Sufferers have revealed they have experienced memory loss, breathlessness, fatigue, rashes and nightmares among other lingering symptoms since contracting coronavirus."

Ashland woman says her COVID-19 recovery is slow
By Hans Boyle of the Mail Tribune | Ashland Tidings | July 21, 2020
"Marya Jansen-Gruber still feels exhausted. It’s been months since she contracted something she thinks is COVID-19, and the symptoms haven’t gone away. Last weekend, the Ashland resident experienced what she called a relapse, which has happened repeatedly since she recovered from the worst of the virus in June."
Coronavirus Update: Labelled ‘recovered,' some survivors face a long haul to their former health
The Globe & Mail (Canada) | July 21, 2020
For a cohort of survivors who refer to themselves as long-haulers, using the term “recovered” fails to recognize it takes some patients months to get back to normal
Coronavirus left this 36-year-old ‘recovered’ but gasping for air
By Mary Landers | Bluffton Today | July 21, 2020
While she was never critically ill, Gillespie also hasn’t fully recovered.
“You know, it's like a daily struggle,” she said this month. “Last week was the first week that I got out of bed every day without crying.”
For This COVID-19 Long-Hauler, Talking, Breathing And Swallowing Are Still A Challenge
By Robin Young and Samantha Raphelson | WBUR | July 21, 2020
"Krakower says the strangest thing about his illness was that he would seemingly start to recover, and then his symptoms would come roaring back worse than before."
COVID-19 patients could be at risk for chronic fatigue syndrome: ‘Your whole life can change if you get this’
By Darcel Rockett | Chicago Tribune | July 20, 2020
"As the world continues to watch the number of COVID-19 cases increase (and daily records being broken), patients with myalgic encephalomyelitis, aka chronic fatigue syndrome, want to tell those recovering from coronavirus to listen up."
Why Coronavirus Seems to Be Causing Some People Long-Term Fatigue
By Frances Williams | Life Hacker | July 20, 2020
People who have been seriously unwell and treated on intensive care units can expect to take some months to recover fully, regardless of their ailment. However, with COVID-19, evidence is mounting that some people who have had relatively mild symptoms at home may also have a prolonged illness.

Fauci Warns About ‘Post-Viral’ Syndrome After COVID-19
By George Citroner | Heathline | July 16, 2020
“Brain fog, fatigue, and difficulty in concentrating,” Dr. Fauci said at the International AIDS Conference. “So this is something we really need to seriously look at because it very well might be a post-viral syndrome associated with COVID-19.”
A mild case of COVID-19 is not a mild case of the flu: Long-haulers’ symptoms linger for months, and lasting effects are still a mystery
By Julie Washington | Cleveland | July 12, 2020
"Most long haulers were never sick enough to be hospitalized or placed on a ventilator, so their cases technically count as mild. Yet some keep feeling symptoms for months. Scientists can’t explain why some COVID-19 patients recover in the standard two weeks, and others don’t."
COVID-19 Can Have Long-Term Effects On Lungs, Heart
By Kara Manke | Futurity | July 9, 2020
"Worrying reports now indicate that the coronarvirus may be capable of inflicting long-lasting damage to the lungs, heart, and nervous system, and researchers are closely watching to see if the kidneys, liver, and gastrointestinal tract may be susceptible to persistent damage as well."
How Covid-19 can damage the brain
By Sébastian SEIBT | France 24 | 7 July, 2020
"Not only does Covid-19 damage the lungs, heart and kidneys, it can also cause severe brain damage – with patients suffering neurological conditions including paranoia and hallucinations, a British scientific study has revealed."
My Covid-19 symptoms have lasted more than 100 days, and I’m not alone. Will they ever end?
By Yochai Re'em | STAT | July 8, 2020
"I write with the hope that even one more patient who has been struggling with prolonged Covid-19 symptoms may not feel so alone. I write with the hope that one more physician, friend, family member, or supervisor may see this article and realize the importance of support since there’s currently a lack of treatment options."
Researchers Examine Recovered Patients For Post COVID-19 Fatigue Syndrome
By Riya Baibhawi | Republic World | 7th July, 2020
"As the world continues to reel under the effects of the COVID-19 pandemic, most people testing positive for the infection experience it as a short-term illness. However, recent evidence emerging out of a significant minority of recovered patients underlines possible post COVID-19 fatigue."
Meet the 'long-haulers': A growing chorus of coronavirus patients have had symptoms for more than 100 days
By Aria Bendix | Business Insider Australia | July 4, 2020
"Most of these patients’ infections have drastically upended their lives. They have dealt with chest pain, shortness of breath, nausea, heart palpitations, loss of taste and smell, and other prolonged symptoms for months. Some are facing unemployment or having to file for disability as they stare down the barrel of chronic illness. Others have struggled to care for their children or family members."
Register for our free 28-Day trial where you can watch lots of videos about how to recover, and access our Member's Area. Or if you are ready to Buy Now, click here
Discover How The Gupta Program Can Support Your Recovery From Chronic Post-COVID-19 Symptoms
It's Not In Your Head. You Are Experiencing Real Physical Symptoms From A Real Physical Condition.
There Is Growing Evidence That ‘Long Haul’ COVID-19 Patients Are Developing The Neuro-Immune Conditions Such As ME/CFS And Fibromyalgia
Throughout the pandemic, government policy, briefings and the media have overwhelmingly focused on patients in the severe category and those who are tragically passing away from the virus. However, there are many millions of people that have contracted the virus and unless their symptoms were classified as "serious", they are left to manage their debilitating and often frightening symptoms at home, often alone without a support network. Their suffering has become invisible.
The reality is that 10% of people are suffering from post-viral symptoms for at least three weeks and 5% can be debilitated for months.
-The Zoe Covid Symptom Study
Guidelines released by health organizations such as NHS, WHO and CDC state that "mild" COVID-19 symptoms typically resolve within 2 weeks, with more severe cases resolving in 6 weeks. However, emerging accounts from those who are classified in the so-called “mild” category are facing on-going debilitating post-viral symptoms, such as fatigue, brain fog, concentration problems and heightened emotions, for 3 or more weeks.
While some medical professionals are aware of this emerging news, others are not and as a result, patients are being disbelieved and dismissed. This leaves these Covid-19 sufferers vulnerable from a medical, social and employment perspective
Greater awareness is urgently needed as the number of cases continues to climb globally.
We Are Dedicated To Helping To Support The Unseen & Invisible Patients Of This Emerging Health Crisis
An Urgent Message From Chronic Illness Expert Ashok Gupta
Medical professionals, the media and society need to urgently take this seriously. We are on the brink of a devastating secondary pandemic of what we are terming "Chronic Post-Covid-19 Syndrome" or "CPCS", in patients who have been formally classified in the "mild" category.
This syndrome is clearly has a profound effect on the brain and the body. It clearly is offering certain post-viral symptoms in many people. These patients require urgent assistance as they are not receiving the care, medical attention or treatment that is needed. A path myself and my clinic are unfortunately all too familiar with in the cases of other conditions such as ME/CFS, Fibromyalgia and MCS.

What Causes Chronic Post COVID-19 Syndrome?
To find out more, please watch this clip taken from Ashok's recent Facebook LIVE entitled Coronavirus & Chronic Conditions: What You Need To Know

If You Think You May Have Post COVID-19 Syndrome, Please Make Sure you are Checked by Your Doctor. In Addition, here Are 3 Steps You Can Take Right Now To Help Your Health
The Gupta Program Has Over 20 Years Supporting The Healing of Patients with Chronic Conditions Including ME/CFS and Post Viral Fatigue


For over two decades our professional clinic has been supporting patients with chronic conditions to rebalance their nervous systems and immune system using the principles of Neuroplasticity.
Now with the increasing prevalence of patients worldwide that are experiencing an unexpected extended recovery, we knew it was our mission to step up and make our research and knowledge that has supported the healing of thousands of our patients, accessible to those who are suffering from Post-COVID-19 Fatigue Syndrome.
It is imperative that we reach as many sufferers as we can to avoid another wave of ME/ Chronic Fatigue Syndrome and Fibromyalgia cases. These patients need specialist treatment to help guide them through their debilitating symptoms and guidance with brain retraining tools & techniques that can help to deeply rejuvenate their mind and body.
If you think you are suffering from Chronic Post Covid-19 Syndrome we invite you to sign up for our Free, 28-Day trial in consultation with your doctor to see if this treatment is right for you.
Register for our free 28-Day trial where you can watch lots of videos about how to recover, and access our Member's Area. Or if you are ready to Buy Now, click here
Further Information On Our Clinic's Perspective On Chronic Post-Covid-19 Syndrome:
It Is A Common Misconception That People Are Passing From The Actual Virus Itself. In fact, It's Our Own Immune System Over-Responding To The Virus Which Is The Ultimate Cause
In the beginning, COVID-19 generally affects the nose. If our epithelial cells, our immune cells in our nose and the back of the nose, are able to defend against the virus, then it can be fought off then and there. If not, it travels down the back of our nasal cavity into our throat area. Once again, we have our immune system to fight it off at that location. However, if our immune system isn't strong enough and we don't manage to fight it off, it then continues into our lungs, and that's when people experience more severe illness.
Within the Gupta Program Amygdala and Insula hypothesis, our whole body- including our whole nervous system and brain - is designed for survival. So, when our bodies and our brains experience a threat, the number one priority is to defend against that virus or pathogen to ensure survival.
So when it starts invading the lungs, the immune system goes into this hyper response. It believes that, "Because I haven't been able to fight off this virus as it's transported down this respiratory tract, it's becoming more and more serious. Therefore, I need to unleash the best possible immune response that I can. I need to garner all the forces that I can to defend against it because my priority is ensuring survival."
The body enters into a cytokine storm, which is a severe immune reaction where an excessive amount of cytokines enter the bloodstream too rapidly. While cytokines play an important role in normal immune response, if they are released too rapidly it can be life-threatening.
As a result, the body develops pneumonia, which is a severe inflammation of the lungs. As a result, patients find it increasingly difficult to breathe. This is seen especially in more vulnerable types of patients that have a weakened immune system, people who are obese and those who smoke.
It is at this point that the patients life is in danger.
If someone recovers from that, there are a percentage of patients who go on to experience chronic symptoms, even if they experienced a mild version of Covid-19:
The Typical Timeline of Observed Symptom Patterns
Even among the previously fit, healthy and often young
The Evolutionary Basis for Why Covid-19 May Become Chronic
Over millions of years of evolution, our bodies have evolved so we can survive in our environment. Our body’s number one priority is survival! And there are threats that we face that can compromise our survival, and these can be of many different types.
In biology it is called the sympathetic nervous system response. And the opposite of the stress or sympathetic system is called the parasympathetic nervous system, often mediated by the vagus nerve. This is when the body calms down and heals, rests, and repairs itself.
However in the event of COVID-19, even once the virus has been fought off, the immune system and nervous system may have become traumatized, still stuck in hyper-response mode because it still believes it is in danger.
The body creates a unique pattern of defense response. The nervous system and the immune system stay in a traumatized state, a conditioned state. Therefore any mild triggers, for instance, opportunistic infections in the body, related or unrelated anxious experiences that patient is going through or even the symptoms of an overstimulated immune system themselves, become triggers for their own own immune system to keep overspending, to keep still defending against that pathogen, just in case.
And it is this hyper-responsive and hyper-primed state of the nervous system and immune system, that creates the on-going symptoms themselves. The immune system always errs on the side of caution. Because its first priority is survival, it prioritizes that over feeling healthy and strong.
Do You Have A Neuro-Immune Conditioned Syndrome (NICS)?
I call the conditions such as ME/CFS, Chronic Fatigue Syndrome, Post-Viral Fatigue and Associated Conditions that we treat, "Neuro-Immune Conditioned Syndromes” or “NICS”.
These defence responses are all over the body, but I believe that they start off in the brain.
You Have A Real Condition With Real Physical Symptoms Caused By A Traumatic Event On The Brain
The Amygdala and Insula Hypothesis
The Amygdala & Insula Hypothesis a ‘vicious cycle’ that, once triggered by severe stressors in people with certain risk factors can perpetuate neurological overstimulation, physiological dysfunction, and many physical symptoms.
These conditions are real physical illnesses in the body, and they are caused by the effects of a traumatic event on the brain. This causes the brain to go into an extreme survival mode. The brain becomes hypersensitive and hyper-reactive.
It is the brain which is over-triggering the sympathetic nervous system and the immune system. And this is due to something called “conditioning” – It is when our brains learn to do something new, again and again. In the brain, the conditioning may specifically occur in parts of the brain called the insula and the amygdala.
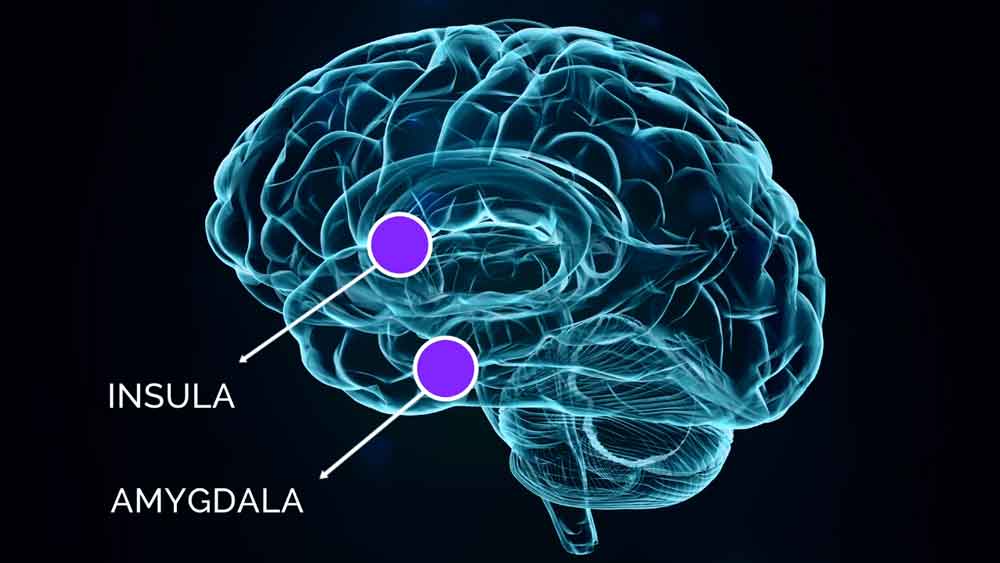
This hypothesis serves as a potential unifying model for the various observations in patients.
The Reason Why Traditional Medicine Finds It Hard To Treat These Conditions...
What Does This Have To Do With Chronic Conditions Such As CFS/ME and Post Viral Fatigue Etc?
I believe all of these conditions are caused by an over-stimulation of these survival responses. These defense responses, are traumatized and over-responding. This means the immune system and the sympathetic nervous system is overstimulated, and it all results in too much inflammation in the body and the symptoms you experience.
How The Symptoms of These Conditions Are Created
Learn more the range of physical, cognitive and emotional symptoms that those with ME/CFS, fibromyalgia, and associated illnesses may experience – explaining how they may be products of amygdala hyper-sensitization.
Amygdala & Insula Retraining (AIR) Within the Gupta Program Breaks This Vicious Cycle By Applying Techniques That Encourage The Brain To Discontinue This Over-stimulation.
Luckily the amygdala and insula constantly communicates with other parts of the brain, and that’s where retraining can take place. Amygdala & Insula Retraining is designed to strengthen the prefrontal cortex and restore inhibitory mechanisms in the insula, anterior cingulate and other associated structures.
The unconscious brain reaction involved in amygdala and insula dysfunction is not normally under a patient’s control, but I believe that my highly specialized “brain retraining” techniques derived from NLP, Timeline Therapy, self-coaching, parts therapy, visualization, breathing, meditation techniques, and others, can target the reaction and control the amygdala and insula, and bring the brain and body back to homeostasis. These are not psychological techniques, but powerful proven neuroplasticity tools to support people's recovery from chronic conditions.
Register for our free 28-Day trial where you can watch lots of videos about how to recover, and access our Member's Area. Or if you are ready to Buy Now, click here